Medical Device Product Lifecycle Management
Protecting installed base revenue through structured lifecycle governance for in-market medical devices — integrating engineering change control, supply continuity, regulatory sustainment, and disciplined value optimization.
Sustaining Medical Devices in a Volatile Market Environment
Once a medical device enters the market, complexity does not decrease — it compounds across regulatory, supply chain, and field performance dimensions.
MedTech manufacturers face persistent lifecycle risks, including:
- Component obsolescence and supplier phase-outs
- Post-market complaints and field performance issues
- Regulatory updates requiring documentation remediation
- Revalidation risk triggered by design or material changes
- Management of Change (MOC) across global markets
- Tariff shifts and sourcing instability
Without structured lifecycle governance, organizations face production disruption, regulatory exposure, unplanned redesign cycles, and revenue discontinuity.
Medical Device Product Lifecycle Management must operate as a disciplined engineering and operational function within production environments — not a reactive support activity.

Structured Sustenance Engineering
and Lifecycle Governance
Sustenance engineering protects product performance, regulatory compliance, and production continuity throughout the commercial lifecycle. Once commercialized, devices require disciplined engineering oversight to prevent performance drift, compliance gaps, and supply-driven instability. Capabilities include:
Engineering change management (ECR / ECO / ECN)
Revalidation Impact Assessment
ISO 13485 – Compliant Controlled Redesign
Integrated Technical File & DHF Governance (DHF, DMR, DHR, TCF)
Field Performance Analysis & CAPA System Alignment
In-Market Performance & Yield Optimization
As a contract manufacturing organization, Syrma Johari MedTech evaluates changes not only from a design perspective but from validated production, tooling capability, yield sensitivity, process-stability, and audit exposure standpoints — minimizing unintended downstream disruption.
Value Analysis &
Value Engineering (VAVE)
Value Analysis and Value Engineering (VAVE) enables structured cost optimization and performance enhancement for in-market devices — without triggering unnecessary regulatory burden. As market competition intensifies, medical device VAVE helps companies differentiate their offerings and adapt products for price-sensitive regions.
As an active manufacturing partner, we understand how architectural decisions impact tooling, validation, and production stability — enabling disciplined value optimization without compromising regulatory standing.
The objective is not cost reduction alone — it is margin protection with regulatory continuity.
Product gap analysis and risk identification
Function-cost-worth analysis grounded in manufacturability
Component rationalization and sourcing alternatives
Performance upgrades through material or subsystem optimization
Engineering-led redesigns requiring controlled requalification
Proactive Component Obsolescence Management
Component end-of-life (EOL) and supplier discontinuations are among the most significant lifecycle risks in medical devices.
Our obsolescence management framework includes:
Engineering, regulatory, and manufacturing teams collaborate to ensure obsolescence mitigation does not introduce unintended revalidation exposure.
Structured BOM scrubbing and lifecycle monitoring
YTEOL & Supplier lifecycle risk analysis
Critical Component Dependency & Single-Source Risk Evaluation
Alternate Component Identification & Qualification Planning
Last-Time-Buy Strategy & Inventory Buffer Planning
Controlled Engineering Change & Revalidation Execution
Regulatory submission support for design modifications
Resilient Supply Chain Governance
Sustained lifecycle performance depends on disciplined global supply chain oversight aligned with production reality and regulatory obligations.
Capabilities include:
- Supplier assessment and ISO 13485–aligned qualification
- Lot-level traceability and SAP-based inventory systems
- Long-lead-time management and strategic stock planning
- Multi-region sourcing strategies
- Continuous supplier performance monitoring
- Risk-based sourcing diversification
Manufacturing-grounded lifecycle management ensures supply continuity decisions reflect real production constraints and regulatory obligations.
Post-Market Regulatory Compliance & Governance
Regulatory sustainment extends far beyond initial market approval — requiring continuous alignment between design changes, field performance data, and global submission requirements.
Lifecycle regulatory support includes:
- DHF remediation and documentation updates
- Ongoing risk management maintenance
- CAPA alignment with field performance data
- Labeling and packaging updates
- Audit readiness preparation
- Submission support for design changes
Change management is structured to preserve compliance continuity while minimizing requalification burden

Manufacturing Led
Lifecycle Ownership
Unlike advisory-led PLM providers, Syrma Johari MedTech executes lifecycle programs within active, validated production environments.
As a medical device contract manufacturer, we understand:
01
Tooling and process validation impact
02
Production yield sensitivity
03
Supplier transition realities
04
Revalidation timelines
05
Regulatory audit implications
Lifecycle management decisions are therefore grounded in operational reality — not theoretical optimization.
This manufacturing-centric ownership model strengthens product longevity, production stability, and global market continuity.

Why Syrma Johari MedTech for Lifecycle Management
- Integrated engineering, manufacturing, and regulatory oversight
- Structured obsolescence governance
- Controlled change management frameworks
- Manufacturing-informed value engineering
- Global regulatory sustainment support
Medical Device Product Lifecycle Management is executed as a disciplined operational function — embedded within engineering, manufacturing, and regulatory systems.
We do not manage lifecycle as a service line — we manage it as a responsibility to protect your installed base, regulatory standing, and long-term production viability.
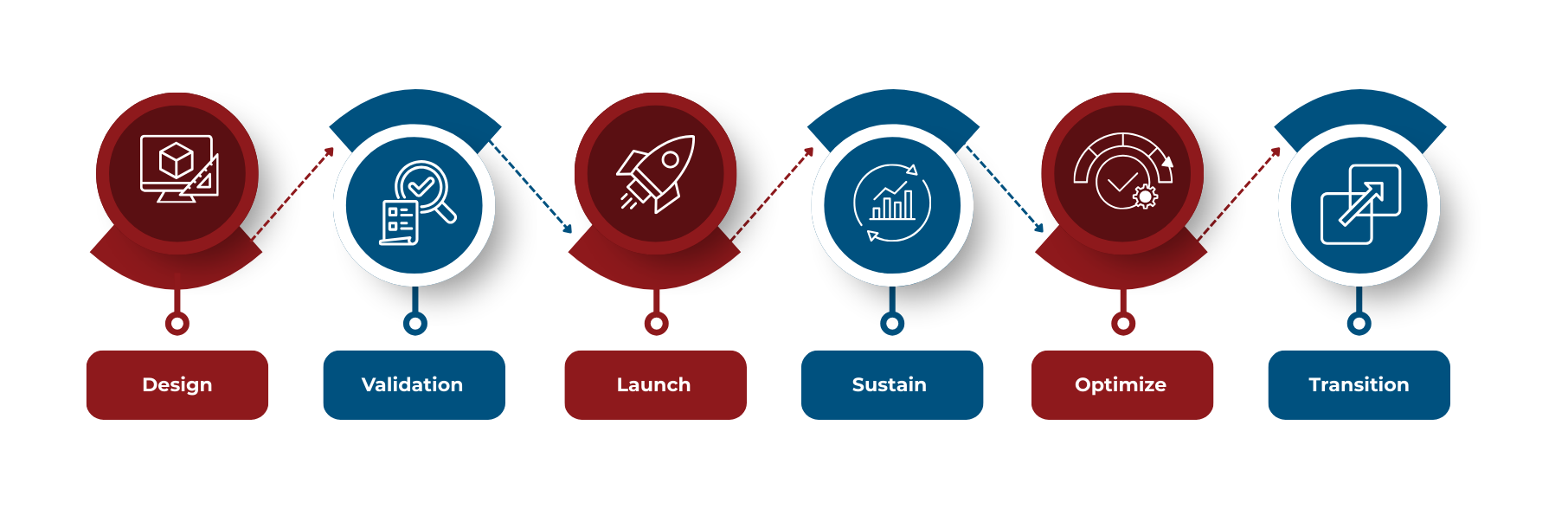
Integrated Lifecycle Governance
Across the Product Continuum
Success Stories
Precision Manufacturing Support for Advanced Endoscopy Systems
Delivered precision manufacturing, quality control, and process optimization to support high-performance endoscopic platforms.
Multi-Generation Redesign & Cost Optimization of a High-Speed IVD Homogenizer Platform
Multi-generation engineering and manufacturing optimization of a pre-analytical homogenization platform achieving ≤40-second lysis, clinical-grade reproducibility, and traceability aligned with global IVD and life sciences requirements.
Strengthen Product Continuity
Across the Lifecycle
Engage Syrma Johari MedTech to evaluate lifecycle governance, obsolescence risk, engineering change readiness, or regulatory sustainment strategies for your in-market medical devices.
Information Center
What is Medical Device Product Lifecycle Management?
Medical Device Product Lifecycle Management (PLM) is the structured governance of in-market devices to maintain performance, compliance, and production continuity. It typically includes sustenance engineering, engineering change control, obsolescence management, supply chain continuity, and post-market regulatory sustainment.
Why is obsolescence management critical for medical devices?
Component EOL and supplier phase-outs can disrupt production and trigger redesigns that require controlled verification, validation, and documentation updates. Proactive obsolescence management reduces disruption by monitoring lifecycle risk, qualifying alternatives, and planning redesign and requalification within ISO 13485-aligned controls.
How do post-market complaints impact lifecycle engineering?
Post-market complaints and field performance trends may require corrective actions, risk file updates, and engineering changes. Lifecycle engineering ensures issues are evaluated systematically, linked to CAPA where applicable, and executed through controlled change workflows to protect compliance and product continuity.
What is revalidation risk, and why does it matter?
Revalidation risk is the likelihood that a design, material, supplier, or process change will require partial or full verification/validation and may impact regulatory documentation. Managing revalidation risk is essential to prevent unplanned testing cycles, remediation of documentation, and production instability.
How do you manage Management of Change (MOC) for global markets?
MOC is managed through structured change control (ECR/ECO/ECN), risk-based impact assessment, and controlled updates to DHF/DMR/TCF as applicable. Changes are planned to maintain traceability, preserve compliance, and align with market-specific regulatory expectations.
How is VAVE applied in lifecycle management without compromising compliance?
Lifecycle VAVE focuses on engineering optimization that preserves performance, safety, and compliance integrity. Activities are executed through controlled change processes, risk reassessment, and defined verification/validation plans to ensure improvements do not introduce unintended regulatory exposure.
What makes Syrma Johari MedTech different from advisory-led PLM providers?
Syrma Johari MedTech executes PLM within active manufacturing environments. This means lifecycle decisions consider tooling, process validation, yield sensitivity, supplier transition realities, and audit implications — ensuring recommendations are grounded in production and compliance realities rather than theoretical optimization.
When should an OEM engage you for PLM support?
PLM engagement can begin at any stage — for recurring field issues, component obsolescence risk, supplier transitions, regulatory updates, or product redesign initiatives. Early engagement is particularly valuable when changes may trigger revalidation or market-specific documentation updates.
COMPANY
- About Us
- Board Members & Leadership
- Certification and Awards
- ESG Initiatives
- Career
LEGAL
- CSR Policy
- Privacy Policy
- Terms & Conditions
CONTACT US
Business Inquiry
© 2026, Syrma Johari MedTech Ltd. All rights reserved.
